Dr. Gerald H. Smith
The term Craniodontics has been coined by this author to focus attention on the fact that use of dental orthopedics/orthodontics or any restorative dental procedure that directly changes the occlusion will affect the alignment of the 22 cranial bones (excluding the 6 ear ossicles). The effectiveness of dental orthopedics in expanding the maxillae both transversely and sagittaly is well documented, however the time has come when dental practitioners must look beyond the parameters of the teeth and alveolar bone to the highly functional cranial system.
In order for cranial bone motion to occur there has to be flexibility of the cranial vault as well as expansion and contraction joints. As stated in the 29th British edition of Gray’s Anatomy, bones derived from membrane, function like membrane throughout life. The squama portion of the occipital and temporal bones as well as the paired parietal and frontal bone structures is derived from membrane. In addition, living bone is saturated with blood, which further enhances inherent flexibility. Dr. John Upledger et al.,1 in the early 1960’s, documented histologically in human cranial bone specimens (taken from living adult skulls at the time of brain surgery) that sutural areas contain blood vessels, nerve plexuses, connective tissue, Sharpey’s fibers and red blood cells. Further substantiation of sutural viability in adult skulls comes from the work of the internationally known anatomist, Dr. Marc Pick. His 150 plus cranial dissections unequivocally document that the dura mater that surrounds the brain provides connective tissue extensions, which pass through the sutures to form the outer periostial layer, which surrounds the skull bones.2 Throughout the cranium there are architectural design alterations of the bevels that exist along sutural lines. These sutural variations enable hinge-like, sliding and pivotal actions. Researchers describe sutures as having the potential for micro-motion as a means of responding to biomechanical forces and stresses, which occur in vivo.3
Retzlaff and other researchers in their “gross and microscopic examination of the parieto-parietal and parieto-temporal cranial sutures obtained by autopsy from seventeen human cadavers with the age range of seven to seventy-eight years shows that these sutures remain as clearly identifiable structures even in the oldest samples. In no instance was there evidence of sutural obliteration by ossification. There are morphological changes in both the cranial bones and sutures which can be correlated with the aging process.” Retzlaff and co-workers suggest cranial suture design as appears within skull bones can have movement at any age. Hubbard and other researchers found “that cranial sutures are slightly more compliant to flexure about an axis along the sutures than the ‘equivalent’ layered cranial bone structures.” Their clinical observation revealed greater movement in the sutures of both embalmed and unembalmed skulls. Based on their findings it would be safe to imply that the living cranium would exhibit an even more degree of flexibility than the sutures in vitro. The viability of the cranial suture as a dynamic structure is well documented in the literature. 6,7,8,9,10,11,13,14,15,16 In the total scheme of body design, cranial sutures function to join other cranial bones together but primarily serve as expansion-contraction joints to allow accommodation for changes in meningeal, muscle and fascial tensions, respiratory and cardiac rhythms and alterations in both cerebrospinal and blood pressure.
The primary respiratory system (pumping action of the brain, cerebrospinal fluid, cranial nerves and dural membrane system) lies within this cranial system and is directly influenced every time the screw is turned on a functional orthopedic appliance. Even placement of a simple bend in an arch wire or attachment of a chain elastic or use of an inter-arch elastic will cause changes in dural membrane tension and cranial bone alignment. All mechanical tensions placed on the teeth will be reflected into the cranial system and if used by design can serve to correct cranial lesions and improve the patient’s quality of life. These various cranial lesions can be diagnosed by means of manual palpation and partially by radiographic analysis (because of its two-dimensional limitations). By using four cranial indicators a road map is provided of where you are before, during, and after treatment. This simple system allows one to easily monitor the course of treatment and to determine when treatment is completed.
Thanks to the clinical research of Drs. Darick Nordstrom, Bob Walker, Granny Langly-Smith, Gaery Barbery, Jim Carlson, Runar Johnson, James Jecmen, and others a level of knowledge now exists that links the occlusal planes (transverse, sagittal, and vertical) and malocclusions with specific misalignments of the cranial bones and accompanied dural membrane tension. This integration has now raised the level of dental orthopedics/orthodontics to a higher standard of care.
Radiographic documentation validates the effects of cranial manipulation
Because of the lightness of touch required for cranial techniques some inexperienced practitioners have termed cranial therapy hocus-pocus or spiritual. Uninformed evaluation leads to misinterpretation. It is impossible for me to term hocus-pocus the gentle, caring touch of thousands of experienced and respected dentists and therapists who produce on a daily basis clinically effective results with cranial therapy. A convenient and scientifically reproducible technique, DORA (Dental Orthogonal Radiographic Analysis- AAFO Journal, Vol. 14, Number 3, May/June/July 1997), has now been established by this author. With the DORA system, practitioners can now scientifically document transverse structural changes that result from cranial releases. This diagnostic system helps establish cranial manipulation as a valid treatment modality within the scope of dentistry.
Case. Mattie S. had headaches for 35 years and deep right thigh pain for the past three years. The head pain started when she was a child. After being thrown from a wagon she collided with a fence. No medication, chiropractic or physical therapy resolved the patient’s problem during the 35-year period. Cranial manipulation was provided by releasing the sphenoid bone by bilaterally unwinding the external and internal pterygoids. This author followed his standard cranial treatment protocol. Following the one-hour cranial manipulation session, the head and thigh pains totally resolved. The patient exhibited a remarkable increase in vertical jaw opening and decompression between the atlas and axis vertebrae. These changes are well documented in the pre and post radiographs taken one hour apart.
Pre-Treatment P-A View
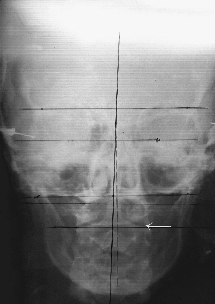
One hour post initial exam
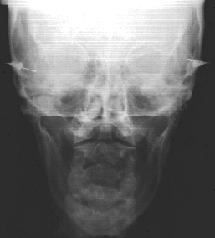

Pterygoid Sling By sequentially releasing the cranium and associated muscle attachments the cranial mechanism can be effectively released. Since the pterygoids, which attach to the lateral pterygoid plates, represent major masticatory muscles they will exert a strong influence on the entire craniosacral system via the tension transmitted to the dural membrane system. The pterygoid sling, which is comprised of the internal and external pterygoid muscles, is directly affected by distortions of the maxillae (transverse and sagittal cants) and malocclusions. When the maxillae becomes transversely canted it directly affects the position of the sphenoid. The sphenoid articulates directly with 14 other cranial bones (occiput, frontal, 2 parietals, 2 temporals, 2 malars, 2 ethmoids, palatine, vomer, and 2 maxillae). The sphenoid articulation with the other 14 bones of the skull represents a 50% direct influence on any changes that occur. In addition, between the sphenoid and the temporal bones, 92% of the cranial nerves pass either in close proximity or through these two bones. Furthermore, the sphenoid bone has extensive dural membrane attachments within the skull and houses the pituitary gland. Torsions or sidebend lesions will greatly influence the dural tube, spine, sacrum, pelvis and potentially the endocrine system. An occlusal discrepancy as little as the thickness of two sheets of typing paper can be adequate to perpetuate chronic pain. The following case study Drs home the significance of this fact.
Case: Mark B. is a 47-year old male who had been suffering fourteen years with upper cervical and low back pain. In 1984, he had accidentally fell two stories through an unguarded elevator shaft and impacted on a cement slab. He suffered numerous spinal fractures and was not expected to survive let alone ever walk. After a year in a body cast he progressed to enter a rehabilitation program and managed to relearn to walk. Various therapies were used to help alleviate the neck pain but to no avail. Fourteen years after the original incident, the patient was referred to me for Craniodontic evaluation. A cranial, dental and Dental Orthogonal Radiographic Analysis was performed. The sphenoid was noted to be low on the right along with compression between the atlas and axis vertebrae. The transverse occlusal plane was canted high on the right and also lacked vertical support on the right (reason for the low sphenoid). Treatment consisted of extensive cranial manipulation, micro-current stimulation and posterior occlusal support in the form of overlay resins. Three resins were placed on the maxillary posterior right side. Within 24 hours the pain started subsiding in the atlas-axis area and within six weeks the low back pain reduced by 75%. The following pre and six-week post radiographs document the impact of correcting a slight cant and vertical deficiency equivalent to two thickness of typing paper.
Pre=Tx Radiograph
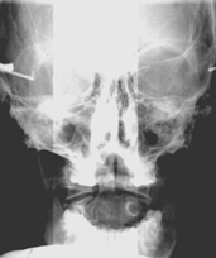
Six week Post-Tx
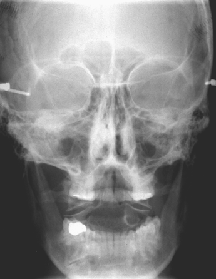
Relationship of dental malocclusions and specific cranial faults
The Class II Division I malocclusion presents itself with a high palatal vault. This distortion results from the vomer bone being pulled upward with a sphenobasilar extension type lesion. Correction of the orthopedic/dental malocclusion helps corrects the cranial distortion.
Sphenobasilar Extension
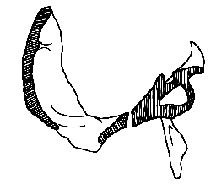
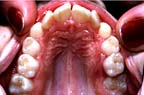
High palate is due to sphenobasilar extension
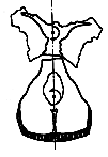
Sphenobasilar Flexion

Low palate is due to sphenobasilar flexion
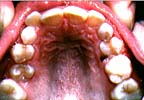
The typical Class II Division II malocclusion exhibits a flexion type cranial lesion. Since the vomer bone directly connects the hard palate with the rostrum of the sphenoid bone, cranial lesions will be reflected as a flat palatal distortion.
A sidebend lesion will be corrected when a sagittal force is appropriately applied. Use of acrylic functional appliances that contact the palate and restrict cranial motion will prevent the release of the cranial bones. Only a lightwire functional appliance system, like the ALF or heavy wire Kernott, can address these issues.
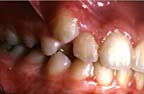
| A right sidebend lesion usually results in a dental malocclusion that manifests itself clinically as an arch length deficiency resulting in a blocked out tooth on the lesion side. |
In light of the validity of these integrated concepts and proven practicality of their clinical use, the indiscriminate application of force via orthopedic appliances and conventional orthodontic braces can no longer be accepted as standard of care. Architectural concepts dictate that the foundation of any structure must be level prior to the start of construction. Since the maxillae represents the anterior 2/3 of the base of the human skull and in essence its foundation, it too must be leveled prior to beginning orthodontic treatment. Albert Einstein defined insanity as “doing the same thing over and over again and expecting a different result.” We can no longer continue striving for better results using the same old concepts and appliances. The cranial road map must be read and used to govern treatment if dentistry is to progress beyond the mechanistic model and transcend into the new technology offered by biologic dentistry.
References
- Upledger, John E., D.O., Retzlaff, Ernest W., Ph.D. and Vredevood, M.F.A.: “Diagnosis and Treatment of Temporoparietal Suture Head Pain”, Osteopathic Medicine, pp. 19-26, July 1978.
- Information obtained through personal communications.
- Blum, Charles.: “Biodynamics of The Cranium: A Survey”, J. Craniomandibular Practices, Vol. 3, No. 2, pp. 164-171, 1985
- Retzlaff, Ernest G., et al.: “Light and Scanning Microscopy of Neuraxis in Human Cranial Sutures and Associated Structures,” Anatomical Records – 93rd Session of the Association of Anatomists, p. 154-A, 1980.
- Hubbard, R. P.: “Flexure of Layered Cranial Bone, J. Biomechanics, Vol. 4, pp. 351-363, 1971.
- Michael, David, K., and Retzlaff, Ernst, W.: “A Preliminary Study of Cranial Bone Movement in the Squirrell Monkey, The J. Amer. Osteopathic Assoc., Vol. 74, May 1975.
- Tettambel, Melicien, et al.: “Recording of the Cranial Rhythmic Impulse,” The J. Osteopathic Assoc., Oct. 1978.
- Upledger, John E., D.O., Retzlaff, Ernest W., Ph.D. and Vredevood, M.F.A.: “Diagnosis and Treatment of Temporoparietal Suture Head Pain,” Osteopathic Medicine, pp. 19-26, July 1978.
- Babler, W. J., Persing, J. A.: “Experimental Alteration of Cranial Suture Growth: Effects on the Neurocranium, Basic Cranium, and Midface,” Factors and Mechanisms Influencing Bone Growth, Alan R. Lias, Inc., New York, NY 10011, pp. 333-345, 1982.
- Behrents, R. G., Carlson, D.S., Ardelnous, T.: “In Vivo Analysis of Bone Strain About the Sagittal Suture in Macatta Mulatta during Masticatory Movements,” J. Dent. Res., Vol. 57, No. 9-10, pp. 904-908, 1978.
- Meikle, M. C., Sellers, A., Reynolds, J. J.: “Effects of Tensile Mechanical Stress on the Synthesis of Metalloproteinases by Rabbit Coronal Sutures in Vitro,” Calcif. Tissue Int., Vol. 30, pp. 77-82, 1980.
- Meikle, M. C., et al.: “Rabbit Cranial Sutures in Vitro: A New Experimental Model for Studying the Response of Fibrous Joints to Mechanical Stress,” Calcif. Tissue Int., Vol. 28, pp. 137-144, 1979.
- Retzlaff, E., et al.: “Aging of Cranial Sutures in Macaca Nemestria,” Anatomical Records—91st Session of the Association of Anatomists, p. 520, 1978.
- Retzlaff, Ernest, et al.: “Aging of Cranial Sutures in Humans,” Anatomical Records—92nd Session of the Association of Anatomists, p. 663, 1979.
- Foley, W. J., Kokich, V. G.: “The Effects of Mechanical Immobilization on Sutural Development in the Growing Rabbit,” J. Neurosurg., Vol. 53, pp. 794-801, 1980.
- Todd, T. Wingate and Lyon, D. W.: “Cranial Sutural Closure—Its Progress and Age Relationship, Part I-IV,” Am. J. Phys. Anthrop., Vol. 7, pp. 324-384, Vol. 8, pp. 23-71, pp. 149-168, 1924-25.

